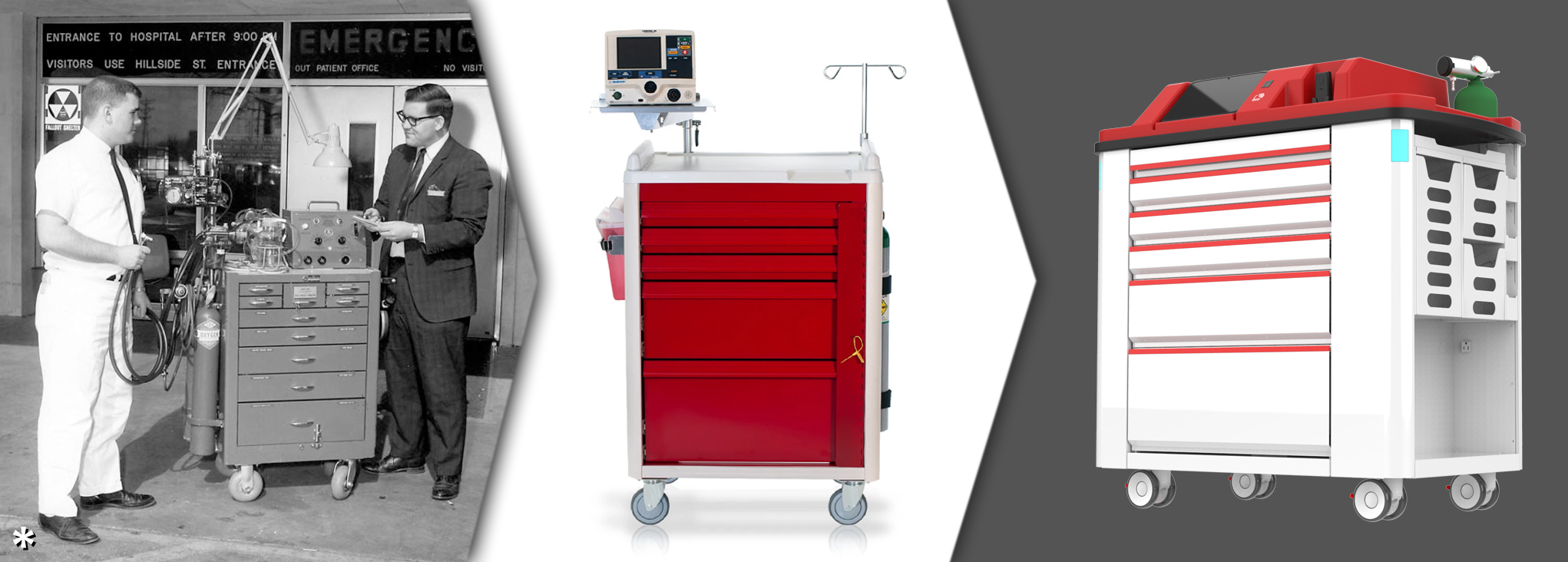
When a Code Blue is called, every second counts. In fact, each minute of delay in resuscitation can lead to a 7 – 10 percent drop in successful in-hospital cardiac arrest (IHCA) outcomes.1 Crash carts, also known as resuscitation carts or emergency carts, are designed to help clinicians make the most of every critical moment.
Providing quick access to the life-saving medication, supplies, and equipment that cardiac arrest patients need, these mobile, all-in-one emergency care kits are like an insurance policy: They sit ready and waiting until a code is called, at which point they are thrust into action and become absolutely essential for survival. That’s why they’re required in virtually every treatment area of every hospital across the United States.
But when and how were these now ubiquitous units first developed? How have they changed since? And in the midst of so much evolving healthcare technology, what does the crash cart of tomorrow look like? Keep reading to find out.
History of the Crash Cart
Like many major inventions, the idea for the crash cart seems to have struck multiple innovators around the same time — in this case, the early 1960s.
This makes perfect sense considering modern resuscitation practices (i.e. combining CPR with medications and devices such as the defibrillator) started to become the standard of emergency care in the late ‘50s. Responders needed a way to access all of these resources quickly, so they started consolidating them into purpose-built mobile storage units.

1969 Crash Cart: Image from Aubrey Patterson/American Association for Respiratory Care’s Virtual Museum
Late 1950s defibrillator: Image from American Association for Respiratory Care’s Virtual Museum

1962 – Bethany Medical Center’s Cardiac Cart2,3
The earliest known version of what we would now consider a crash cart was developed in 1962 at Bethany Medical Center in Kansas City, Kansas by the same team that coined the term “Code Blue.” The “cardiac cart” was fabricated by the father of one of the team’s physicians and contained a bag valve mask, defibrillator paddles, bed board, and endotracheal tubes.
1965 – Dr. Joel J. Nobel’s MAX Cart4
Somewhat concurrently, Pennsylvania Hospital Resident and patient safety advocate Joel J. Nobel, MD (1934 – 2014) began developing the MAX cart. MAX doubled as a treatment table and life-support system, featuring medication drawers, storage cabinets, security features, and built-in equipment such as a pneumatic cardiac compressor and electrocardiograph. It even recorded data, such as voice and ECG readouts, facilitating event analysis and improvements over time.

In 1965, Dr. Nobel patented MAX, and so is widely credited as the official inventor of the crash cart. Three years later, he founded the Emergency Care Research Institute (ECRI), an independent, nonprofit organization still dedicated to improving the safety, quality, and cost-effectiveness of care across all healthcare settings worldwide.

1967 – Nurse Anita Dorr’s Emergency Nursing Crisis Cart5–7
Before MAX or any crash cart reached widespread adoption, at least one more resuscitation enthusiast independently developed another well-known prototype. While supervising the Emergency Department of E.J. Meyer Memorial Hospital (now Erie County Medical Center) in Buffalo, New York, nursing legend and activist Anita Dorr, RN, FAEN (1915 – 1972) realized it was taking far too long to gather cardiac and respiratory arrest treatment resources.

Dorr worked with fellow nurses to compile a list of emergency response medications, supplies, and equipment, then enlisted the help of her husband to design and build the “Emergency Nursing Crisis Cart” in their garage in 1967.
In some ways, the cart Nurse Dorr created more closely resembles the crash carts still in use today, as it enabled more flexible configuration.
Although Nurse Dorr was never able to patent her cart design, she went on to co-found and preside over the Emergency Department Nurses Association (now the Emergency Nurses Association) in 1968, among many other achievements.

How Crash Carts Are Used Today
Eventually, Dr. Nobel’s MAX cart and others like it were replaced by a simpler design — basically a medical grade automotive tool cart that has changed very little over the subsequent 50-plus years.
But during that time, crash cart use has spread far and wide, helping clinicians save countless lives across the globe. Today, crash carts can be found — and in fact are often required, depending on state laws — in any facility that treats patients whose condition may suddenly deteriorate. This includes hospitals, emergency rooms, urgent care centers, outpatient surgery centers, and cardiac stress testing centers.

Common Crash Cart Contents
There are many ways to set up and organize a crash cart. But regardless of how they are configured, crash cart contents typically include8:
- Equipment & supplies, such as:
- Monitor & defibrillator
- Airway equipment, such as bag valve masks, oral/nasal airways, oxygen masks, & cannulas
- IV/IO access equipment, including angiocaths, IV tubing and fluid, and an IO drill and needles
- Plus medications for treating:
- Cardiac arrest (epinephrine and amiodarone)
- Cardiac dysrhythmias (adenosine, diltiazem, beta blockers, and atropine)
- Allergic reactions (epinephrine, methylprednisolone, and diphenhydramine)
- Myocardial infarction (aspirin and nitroglycerin)
The Crash Cart Use Cycle
Crash carts typically cycle through seven key phases or steps. Each is vitally important to ensure Code Blue event readiness, high-quality care, and optimal outcomes.

- Setup & configuration (only occurs once): Carts should be outfitted with all the appropriate emergency care medication, supplies, and equipment, organized per hospital policy.
- Placement: To ensure a quick, coordinated response, the cart should be placed in a location that is central to and easily accessible by the designated members of the code team assigned to a specific care area.
- Cart checks: These inventory and compliance inspections should be performed and documented regularly to ensure every cart is code-ready at all times. Ideally, cart check forms and processes should be standardized across the hospital.
- Code initiation: The moment a code is called, the cart must be rushed by a designated care team member to the patient. All equipment should be unplugged from the wall before moving to avoid accidents or damage, and cart contents should be secured and organized in a way that supports rapid mobility.
- Patient care: Clinicians must be able to access all resources and reference sheets quickly and easily during the code response to ensure patients get the care they need the instant they need it.
- Documentation: During the code response, a scribe should document interventions as they take place and note what resources are being used in real time. Ideally, documentation supplies should be stored on the cart. This information is needed for optimizing care in the moment, keeping complete patient records, debriefing to improve outcomes over time, and managing inventory.
- Restocking: Reconciliation and replenishment should occur as soon as possible after the event, taking into account documentation of all resources used during the code. Once the cart is restocked, the use cycle begins anew with “Placement.”
Future-focused Crash Cart Advancements
Overdue for Innovation
The future of the crash cart is inextricably tied to the future of Code Blue care. And just as IHCA outcomes are in dire need of improvement,9,10 so are many aspects of decades-old crash cart design and operations.
- Readiness awareness: There is no way to know definitively at-a-glance whether typical crash carts are code-ready. Response teams have to trust that all resources are present, not expired, charged, and stored in their appropriate locations on the cart. Unfortunately, this is often not the case, resulting in treatment delays and compliance issues.
- Manual processes: From inventory management to cart checks to event documentation, most crash cart processes are still performed via pen and paper. This increases the likelihood of errors, makes reporting and administration extremely difficult, and eats up a significant amount of clinicians’ valuable time.
- Disorganized storage: Because cart configuration is typically not standardized, carts can become cluttered and disorganized, making it harder for response teams to find what they need to treat patients quickly.

- Mobility issues: With many carts, equipment such as defibrillators and suction pumps must be plugged into a wall outlet to charge between codes. In the urgent rush to transport the cart once the code is called, clinicians often forget to unplug these items, which can then be pulled off the cart, causing damage and treatment delays.
- Lack of integration with other systems: Because crash carts typically don’t interface with EHR, central supply, or pharmacy systems, they often become a troublesome gap for hospital inventory management and reporting.
Introducing the All-in-one Solution from Nuvara®

The EMMIT™ Emergency Care System represents the biggest leap forward in crash cart technology since the device’s invention. That’s because EMMIT is so much more than a crash cart — it’s the only comprehensive system of hardware, software, and services that addresses all the challenges above and more, delivering:
- Digital visibility into the presence and status of medications, supplies, and equipment on the cart
- Real-time awareness of the emergency response readiness level of the entire hospital
- Electronic processes for cart checks, inventory management, event documentation, & reporting
- Next-gen storage that helps clinicians consolidate resources, organize configuration, and easily access all emergency care resources
- Quick-to-care design with readiness indicator lights, a breakaway plug, and quick-start software
- Integration with other systems, including EHR, central supply, pharmacy, and reporting
Related Articles
Meet the Crash Cart of Tomorrow, Today
Crash carts are critical for hospital emergency care. And thanks to technologies like the EMMIT Emergency Care System, they now have the power to contribute even more to improved IHCA performance and outcomes. Contact us to learn more about what EMMIT can do for your hospital.
*1965 Crash Cart in Featured Image: From Aubrey Patterson/American Association for Respiratory Care’s Virtual Museum
References
-
Simpson KH. 5th Ed. 2. Vol. 97. London, UK: The Resuscitation Council; BJA; 2006. Advanced Life Support.
-
Colby WH. Unplugged: Reclaiming Our Right to Die in America.
-
KUMC History Archives, 1960-1969. Accessed April 21, 2021 at: https://www.kumc.edu/school-of-medicine/history-and-philosophy-of-medicine/kumc-archives/kumc-history/1960-1969.html
-
Crash Cart information article. Accessed April 21, 2021 at: https://en.wikipedia.org/wiki/Crash_cart#:~:text=The%20first%20cardiac%20crash%20cart,bed%20board%20and%20endotracheal%20tubes.
-
Schriver JA, Talmadge R, Chuong R, Hedges JR. Emergency nursing: historical, current, and future roles. Acad Emerg Med. 2003 Jul;10(7):798-804. doi: 10.1111/j.1553-2712.2003.tb00076.x.
-
Fadale JM. As we celebrate: reflections on Anita Dorr and early ENA days. J Emerg Nurs. 2000; 26:31–4.
-
Jezierski M. Profiles: Anita Dorr: her legacy to ENA. J Emerg Nurs. 1996; 22:258–60.
-
ACLS Crash Cart Supply & Equipment Article. Accessed April 21, 2021 at: https://www.acls.net/acls-crash-cart.htm
-
Holmberg MJ, Ross CE, Fitzmaurice GM, et al. Annual incidence of adult and pediatric in-hospital cardiac arrest in the United States. Circ Cardiovasc Qual Outcomes. 2019 July;12:1-8.
-
Virani SS, Alonso A, Benjamin EJ, et al. Heart disease and stroke statistics—2020 update: a report from the American Heart Association. Circulation. 2020 Mar;141:e139-e596.